
Prostate cancer > Treatment options for prostate cancer that has not spread beyond the gland
The long-term picture?
Long-term studies provide information on the prospects of men who have undergone these procedures. While many men want this kind of information, it is important not to take the figures given here too much to heart without discussing your own individual circumstances with your urologist. Progress in medicine means that patients' long-term prospects are improving all the time, and in due course the results of ongoing clinical studies will resolve many controversies.
Active surveillance The likelihood that your cancer will spread depends, as has already been said, on the nature of your cancer (that is, how aggressive it is). For men whose cancer has a low Gleason score (i.e. well-differentiated tumours), the 10-year survival rate is 87%, which means that, after 10 years, 87 men in 100 will not have died from prostate cancer. With more aggressive cancers (those with higher Gleason scores), the survival rate drops considerably (the 10-year survival rate for men with poorly differentiated tumours has been put at 26%). Watchful waiting is often a good option to start with as more active treatment can always be instituted if signs of cancer progression develop.
Radical prostatectomy More than 80% of men who have this operation are alive 10 years afterwards, and 60% are still alive at 15 years. A Scandinavian study compared the long-term outcomes of men who chose active surveillance with those treated by radical prostatectomy. The results suggest that radical prostatectomy is the treatment option most likely to offer a complete cure for younger men, as it physically removes both the cancer and the entire prostate from the body, making recurrence and spread to the bones much less likely. Another study published recently also showed a survival advantage in patients treated with surgery after 8 years of follow-up.
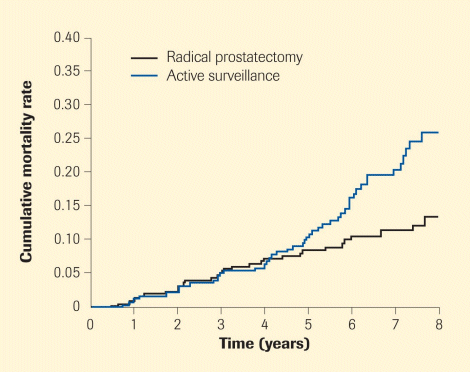 |
| Radical prostatectomy is most likely to offer a better long-term outcome in terms of survival compared with active surveillance. |
Results from a study by Pound and colleagues confirm that 82% of men undergoing radical prostatectomy at Johns Hopkins Hospital in Baltimore (USA) were free of recurrence at 15 years (as determined by PSA measurement). The study also offers some comfort to those men whose PSA level rises years after the operation. As we have already said, after a radical prostatectomy, your PSA level drops to an undetectable level and, if it starts rising again, it can signal cancer recurrence. The data from the study in question indicate that, though this is the case, the cancer spreads in only around one-third of men with an elevated PSA. Furthermore, unless a man had a particularly aggressive cancer (in which case his PSA level would tend to rise relatively quickly after the operation), the spreading cancer would not become life-threatening for several years, and would likely be amenable to treatment with radiotherapy or LHRH analogues.
Radiotherapy At best, the survival rates with radiotherapy are comparable to those associated with radical prostatectomy. Several published studies have put the 15-year survival rates at 40-60% (that is, in a group of 100 men, between 40 and 60 will still be alive after 15 years). Recent data suggest that the ongoing use of LHRH injections or anti-androgens to shrink the prostate ahead of radiotherapy can increase the likelihood that treatment will be successful. The risk of serious side effects with radiotherapy is decreasing as improved technology means that the cancer-destroying rays can be targeted more accurately at the cancer, leaving adjacent structures, such as the rectum, undamaged. Proponents of brachytherapy also report improving results as techniques and patient selection are enhanced. However, problems with potency are still frequently encountered after radiotherapy and, in fact, are much more common when this treatment is combined with hormone therapy.
A sequential rise in PSA after either external beam radiotherapy or brachytherapy does suggest that recurrence has occurred. Although salvage surgery is technically feasible in some cases, it is often difficult and associated with a high complication rate. Sometimes, cryotherapy or high-intensity focused ultrasound (HIFU) can be used to destroy the residual cancer, but more commonly hormone therapy is used.